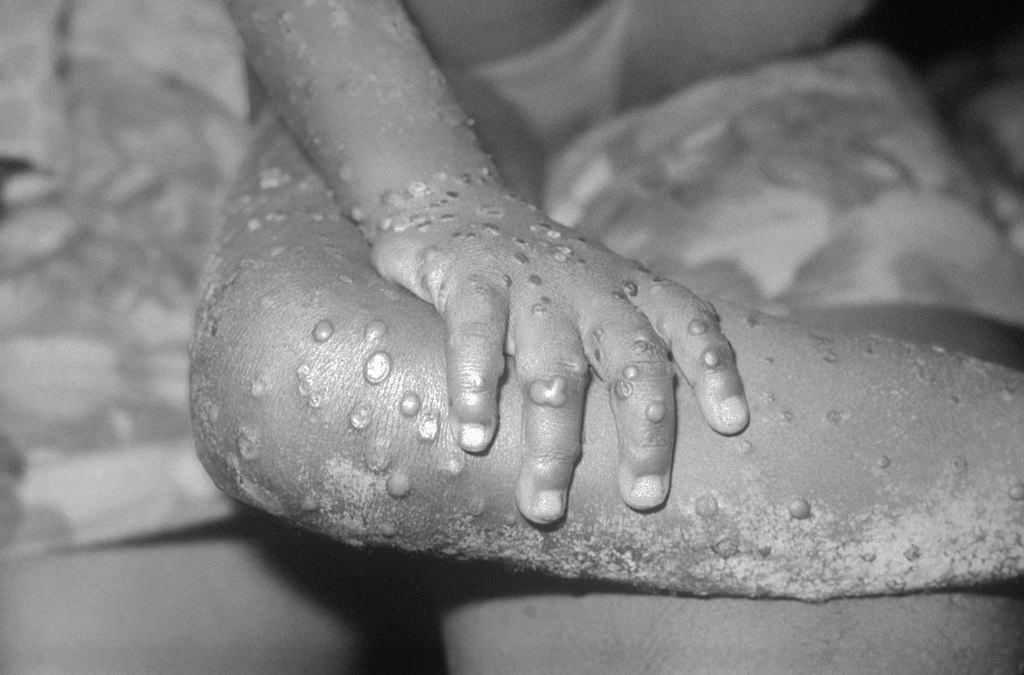
When monkeypox cases in Europe began to decline this summer, researchers’ first question was: Is it real? Some worried that people might not be getting tested because of receding fears of the virus, coupled with strict isolation requirements for patients. “They might be reluctant to be confirmed and be told not to go out at all,” says Catherine Smallwood, monkeypox incident manager at the WHO’s Regional Office for Europe. www.science.org/content/article/monkeypox-cases-are-plummeting-scientists-are-debating-why?
But the decline is now unmistakable. WHO Europe, which reported more than 2,000 cases per week during the peak in July, is now counting about 100 cases weekly. In the Americas, the other major epicentre of the outbreak, numbers have dropped by more than half.
Vaccines, behaviour change among the most affected group—men who have sex with men (MSM)—and immunity after natural infection are all playing a role in that decline, says Erik Volz, an infectious disease modeler at Imperial College London, but how much each factor has contributed is unclear.
The answer is important because it determines the likelihood of a resurgence of the virus. Knowing what has driven down cases so far will also help shape strategies to eliminate the virus outside endemic countries in Africa, a goal WHO Europe is already pushing for.
In the United Kingdom, at least, vaccination campaigns have played a minor role, according to a model published as a preprint this month by Samuel Brand, an infectious disease modeler at the University of Warwick. Monkeypox’s reproductive number—the average number of new infections triggered by an infected person—began to drop by mid-June, even though campaigns only started in July. Several other European countries saw the same pattern.
That leaves behaviour change and immunity from natural infections. A survey conducted by the US Centers for Disease Control and Prevention among MSM in August found about half had reduced their number of sexual contacts. As awareness of the disease increased, people also became more likely to seek diagnosis and treatment early and to avoid sex while they were infectious. The UK Health Security Agency has presented data suggesting syphilis and other sexually transmitted infections declined as well—which would bolster the case for behaviour change.
Immunity acquired through infections in the most sexually active men may be the biggest factor, however. Monkeypox has been affecting mostly MSM and their sexual networks because parts of those networks are densely connected, with some people having a large number of sexual contacts. Rising immunity in that group could limit the virus’s ability to spread.
For Smallwood, that raises a concern: that MSM who feel reassured by the plummeting case numbers may revert to their past behaviour. That’s why vaccination of at-risk groups may now be more important than it was at the peak of the epidemic, she says. Brand agrees; in fact, his UK model suggests that although a slight uptick in cases in the coming months is likely, vaccinations should prevent a real resurgence.

