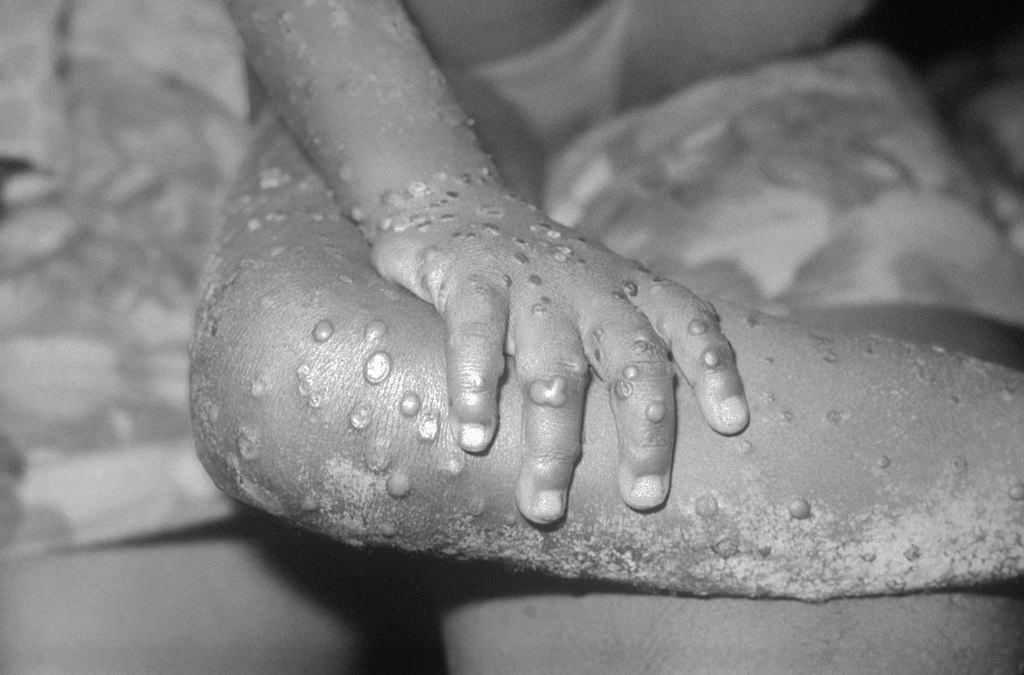
Advisers to the US Centers for Disease Control and Prevention (CDC) has voted in favour of the Bavarian Nordic’s Jynneos vaccine for all adults at risk of mpox during an outbreak. https://www.medscape.com/viewarticle/988606?src=wnl_edit_tpal&uac=398271FG&impID=5194437&faf=1
The panel of outside experts voted unanimously in favour of using two doses of the vaccine, and finalising the interim guidelines provided by the CDC during the mpox outbreak in the United States.
The recommendation of the committee is based on studies that showed vaccine effectiveness of 66%-83% for patients with full vaccination and 36%-86% for partial vaccination with no severe adverse effects.
The intradermal Jynneos injection is the preferred form of administration for adults during the outbreak, but is also approved as a subcutaneous (below the skin) injection.
The panel’s recommendation will give Bavarian Nordic’s vaccine an edge over Emergent BioSolutions’ smallpox vaccine, which last year received approval for expanded use the during mpox outbreak but its use has been largely limited owing to severe side-effects.
Mpox which spreads via close contact and tends to cause flu-like symptoms and pus-filled skin lesions, remains a public health emergency of international concern. Earlier in February the World Health Organization (WHO) retained its highest level of alert for the disease citing continued transmission in some countries.
In the United States, more than 29,000 cases of mpox were reported last year, including two deaths, according to government data.
////
In June 2022, a young man in his 30s severely sick with mpox, was admitted to the Salvador Zubirán National Institute of Health Sciences and Nutrition hospital in Mexico City. Tests showed the patient was also HIV-positive, which he had not known, and that his blood had few critical immune CD4 cells that HIV attacks. The man’s immune system was so weak it could not keep mpox in check and painful lesions kept spreading across his body, eating away at, or necrotizing, the flesh, according to HIV researcher Brenda Crabtree Ramirez, who was on his care team. https://www.science.org/content/article/case-studies-expose-deadly-risk-mpox-people-untreated-hiv?
With no treatments available, his doctors got the hospital’s ethics board to approve a desperate plan: They would transfer blood plasma from a colleague who had been vaccinated in the United States against mpox to the patient, in the hope that the antibodies from the donation might help fight his infection with the poxvirus. The experimental therapy failed—the man died 2 weeks later, one of the first deaths from the disease in Mexico.
Although mpox cases have plummeted globally since then, the outbreak still simmers in Latin America and other locations. A grim report in The Lancet, being presented at a conference in Seattle, which analyses the death last summer in Mexico and the cases of 381 other mpox patients who also had advanced HIV infections, makes clear that the disease poses an enormous risk to those living with uncontrolled HIV. Of the 179 patients with less than 200 CD4 cells per microliter—more than 500 is considered normal—27 have died.
Mpox isn’t just more severe in these immunocompromised patients, says Oriol Mitjà, an infectious disease researcher at the Germans Trias i Pujol University Hospital in Barcelona and one of the study authors, “it’s like a different disease.” In the cases where people had few CD4 cells, mpox’s normally small skin lesions grew into large necrotizing patches and their infection sometimes spread to the lungs or caused severe secondary infections with bacteria.
The Lancet report also contained a warning for physicians: Starting coinfected patients on antiretrovirals for their HIV infection could worsen their mpox. The data presented in the Lancet report are compelling and WHO plans to assemble a group to consider the research team’s recommendation to make mpox an AIDS-defining condition, says Meg Doherty, who heads the program for HIV and other sexually transmitted infections at the agency
////
Every two minutes, a woman dies during pregnancy or childbirth, according to the latest estimates released in a report by United Nations agencies. This report, Trends in maternal mortality, reveals alarming setbacks for women’s health over recent years, as maternal deaths either increased or stagnated in nearly all regions of the world.
“While pregnancy should be a time of immense hope and a positive experience for all women, it is tragically still a shockingly dangerous experience for millions around the world who lack access to high quality, respectful health care,” said Dr Tedros Adhanom Ghebreyesus, Director-General of the World Health Organization (WHO).
The report, which tracks maternal deaths nationally, regionally and globally from 2000 to 2020, shows there were an estimated 287,000 maternal deaths worldwide in 2020. This marks only a slight decrease from 309,000 in 2016 when the UN’s Sustainable Development Goals (SDGs) came into effect. While the report presents some significant progress in reducing maternal deaths between 2000 and 2015, gains largely stalled, or in some cases even reversed, after this point.
In two of the eight UN regions – Europe and Northern America, and Latin America and the Caribbean – the maternal mortality rate increased from 2016 to 2020, by 17% and 15% respectively. Elsewhere, the rate stagnated. The report notes, however, that progress is possible. For example, two regions – Australia and New Zealand, and Central and Southern Asia – experienced significant declines (by 35% and 16% respectively) in their maternal mortality rates during the same period, as did 31 countries across the world.
In total numbers, maternal deaths continue to be largely concentrated in the poorest parts of the world and in countries affected by conflict. In 2020, about 70% of all maternal deaths were in sub-Saharan Africa. In nine countries facing severe humanitarian crises, maternal mortality rates were more than double the world average (551 maternal deaths per 100,000 live births, compared to 223 globally).
“This report provides yet another stark reminder of the urgent need to double down on our commitment to women and adolescent health,” said Juan Pablo Uribe, Global Director for Health, Nutrition and Population at the World Bank, and Director of the Global Financing Facility.
Severe bleeding, high blood pressure, pregnancy-related infections, complications from unsafe abortion, and underlying conditions that can be aggravated by pregnancy (such as HIV/AIDS and malaria) are the leading causes of maternal deaths. These are all largely preventable and treatable with access to high-quality and respectful healthcare.
Community-centred primary health care can meet the needs of women, children and adolescents and enable equitable access to critical services such as assisted births and pre- and postnatal care, childhood vaccinations, nutrition and family planning. However, underfunding of primary health care systems, a lack of trained health care workers, and weak supply chains for medical products are threatening progress.
Roughly a third of women do not have even four of a recommended eight antenatal checks or receive essential postnatal care, while some 270 million women lack access to modern family planning methods. Exercising control over their reproductive health – particularly decisions about if and when to have children – is critical to ensure that women can plan and space childbearing and protect their health. Inequities related to income, education, race or ethnicity further increase risks for marginalized pregnant women, who have the least access to essential maternity care but are most likely to experience underlying health problems in pregnancy.
“It is unacceptable that so many women continue to die needlessly in pregnancy and childbirth. Over 280,000 fatalities in a single year is unconscionable,” said UNFPA Executive Director Dr. Natalia Kanem. “We can and must do better by urgently investing in family planning and filling the global shortage of 900,000 midwives so that every woman can get the lifesaving care she needs. We have the tools, knowledge and resources to end preventable maternal deaths; what we need now is the political will.”
The COVID-19 pandemic may have further held back progress on maternal health. Noting the current data series ends in 2020, more data will be needed to show the true impacts of the pandemic on maternal deaths. However, COVID-19 infections can increase risks during pregnancy, so countries should take action to ensure pregnant women and those planning pregnancies have access to COVID-19 vaccines and effective antenatal care.
The report reveals that the world must significantly accelerate progress to meet global targets for reducing maternal deaths, or else risk the lives of over one million more women by 2030.
/////
Lalita Panicker is Consulting Editor, Views and Editor, Insight, Hindustan Times, New Delhi

