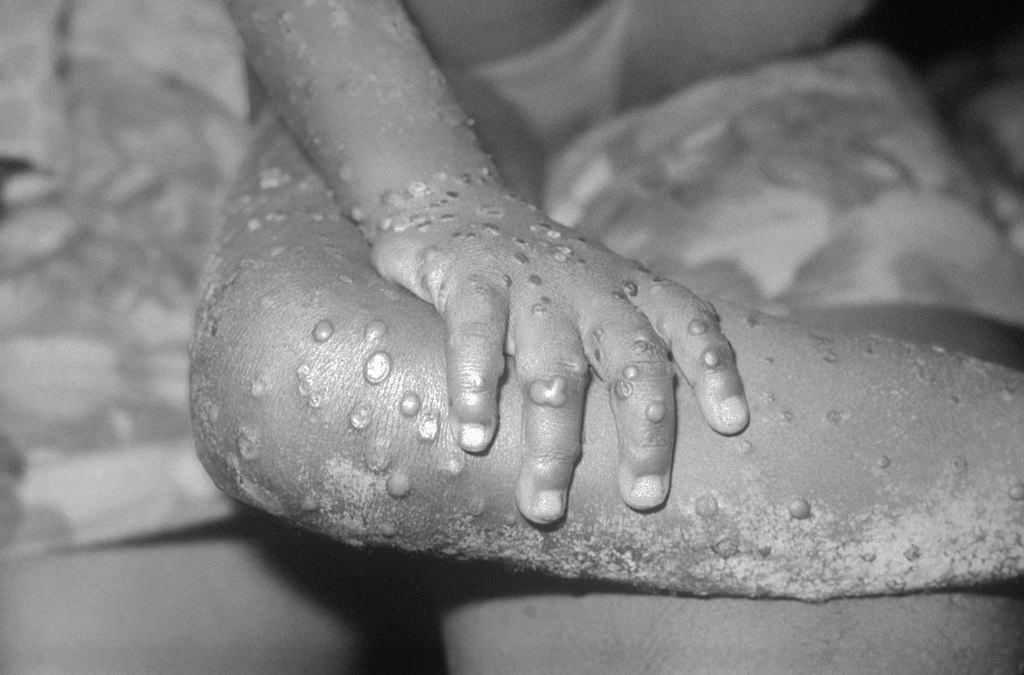
The World Health Organization (WHO) ended the global health emergency for mpox, on 11 May, 10 months after it was declared, as cases have fallen dramatically in Europe and the Americas. www.science.org/content/article/who-ends-mpox-emergency?
Caused by the monkeypox virus (MPXV), the painful and occasionally fatal disease is endemic in Africa, but a new strain surged in other locations last year, sparking WHO to invoke a Public Health Emergency of International Concern (PHEIC), the same type of worldwide alarm that was lifted last week for COVID-19.
The agency’s director-general, Tedros Adhanom Ghebreyesus, said at a press conference in Geneva last Thursday that WHO’s emergency committee monitoring the mpox outbreak recommended ending the PHEIC at a meeting the day before, and that he has accepted its advice.
“That does not mean that the work is over,” Tedros said. “Mpox continues to pose significant public health challenges that need a robust, active, and sustainable response.”
Tedros noted that nearly 90% fewer mpox cases were reported to WHO in the past 3 months compared with the preceding 3 months. In total, WHO has received reports of more than 87,000 mpox cases and 140 deaths from 111 countries, but natural immunity and changes in behaviour appear to have curtailed the disease’s spread.
At the height of the outbreak in the summer of 2022, when the disease was still commonly called monkeypox, more than 7,000 weekly cases
were being reported in the Americas and Europe alone. MPXV, a member of the poxvirus family, is spread by intimate personal contact. In the current outbreak, men who have sex with men (MSM) have been particularly affected. It commonly causes a rash and flulike symptoms and is rarely fatal, but people with severely weakened immune systems are at particular risk of poor outcomes.
Nicola Low, an infectious disease epidemiologist at the University of Bern and the vice-chair of WHO’s emergency committee on mpox, said the committee had “intense” deliberations over lifting the PHEIC, but decided that long-term efforts rather than emergency measures are now the best way to control MPXV.
The challenges are many, however, including a scarcity of vaccines and a lack of data that show how well they work, uncertainty about the modes of transmission in some places, and stigma that imperils those most vulnerable to the disease, especially people living with untreated HIV. Small outbreaks in specific countries also continue, Low noted. “So there is understandable uncertainty about the probability of a large resurgence of infection.”
Several WHO officials pleaded for countries and international groups to make financial commitments to monitor, treat, and understand the disease going forward. “It is clear the recommendation to lift the [PHEIC] in no way means that mpox is no longer an infectious disease threat,” Low said. “What it means is we need to have the international commitments that will enable us to reach the long-terms goals of control and elimination of human-to-human transmission.”
So far such commitments have been lacking, said Michael Ryan, executive director of WHO’s Health Emergencies Programme. Mpox “has been totally neglected during this outbreak [during which] not one dollar was received from donors” to support WHO’s response, he said. He suggested donors slighted the disease because it was largely confined to Africa in the past and predominantly affected MSM in the current global outbreak. “Maybe it’s an issue of the continued prejudice in this world. … It will continue to be a neglected disease. And it may come back. And it may shock us in the future.”
////
Researchers have released the first “pangenome,” representing individuals with ancestry from across the globe. The work could improve the genetic testing for various diseases and even provide new insights into human evolution and biology. www.science.org/content/article/pangenome-hopes-represent-more-diverse-view-humans?
“It’s an exceptional advance,” says Mashaal Sohaila, an evolutionary geneticist at the National Autonomous University of Mexico who was not involved in the project. “It’s making the picture of human genetic variation more accurate and more complete.” When the first human genome was published in 2001, it wasn’t quite finished. It was missing about 8% of its genetic alphabet, which was hard to read with the sequencing technology of the time. Scientists have been adding to this “draft genome” ever since, with the last update, known as GRCh38, released in 2017. Last year, researchers published the most complete human genome to date, one that represents virtually 100% of the total human sequence.
But this complete reference genome, known as T2T-CHM13, still doesn’t reflect the genetic diversity of our species. It doesn’t include the many versions of the same gene, or alleles, that might be present in some population but not others, for example. It’s also missing so-called structural variants—large chunks of DNA that could explain why each one of us is different.
What’s more, because both GRCh38 and T2T-CHM13 are mainly built from individuals of mostly European ancestry, medical tools that use them as a reference might not work for patients of non-European descent. Biological markers that help predict certain kinds of cancer might be more accurate in people from particular parts of the globe, for example, and a genetic marker that helps gauge a person’s risk of coronary heart disease may be vastly underestimating the risk in Black people.
To fill those gaps, Benedict Paten, a computational genomicist at the University of California, Santa Cruz (UCSC), and his colleagues at the Human Pangenome Reference Consortium (HPRC) incorporated genomes collected from 47 individuals and their parents, with the whole group representing every continent except Antarctica. They analysed the genome of each individual in detail, parsing out which portions belonged to each parent. To have a high-quality resolution of each genome, the researchers sequenced long reads of DNA, allowing
them to capture more variations than previous research efforts, the scientists report today in a series of papers published in Nature.
The new pangenome is not only relevant medically, it will also open the doors to more accurate evolutionary genetic studies, Sohail says. With more people now represented, researchers could fill gaps in our evolutionary history, especially in historically understudied parts of the globe.
////
www.science.org/content/article/news-glance-respiratory-disease-vaccine-intensifying-cyclones-shaking-wood-building?
A decades long effort to develop a vaccine against respiratory syncytial virus (RSV), a respiratory pathogen that targets infants and the elderly, succeeded last week when the U.S. Food and Drug Administration (FDA) green-lighted one made by manufacturer GlaxoSmithKline.
The vaccine, the first ever approved, will become available to people ages 60 and older if, as expected, an advisory committee at the U.S. Centers for Disease Control and Prevention recommends it next month. A similar vaccine by pharmaceutical giant Pfizer is also expected to win approval for use in older people this month. And FDA has committed to deciding by August whether to allow use of the Pfizer vaccine in pregnant people, who pass protective antibodies to their new-borns. Annually, RSV kills an estimated 33,000 people ages 60 and older in hospitals in high-income countries. It also kills an estimated 46,000 infants younger than 7 months old, most of them in developing countries.
/////
Rochelle Walensky, who directed the U.S. Centers for Disease Control and Prevention (CDC) through a turbulent pandemic era, will leave her job at the end of June, she announced last week. Walensky took up her post in January 2021 after leading the infectious diseases division at Massachusetts General Hospital. www.science.org/content/article/news-glance-respiratory-disease-vaccine-intensifying-cyclones-shaking-wood-building?
During the COVID-19 pandemic, the CDC was buffeted by criticism, including that it bowed to the political agenda of former President Donald Trump’s administration; after President Joe Biden named Walensky director, she made communications missteps seen as further eroding public trust in the agency. Last summer, she launched a reorganisation that included a focus on making CDC’s public communications better and faster. The timing to nominate a successor is uncertain. Beginning on 20 January 2025, the U.S. Senate will need to confirm any new nominee for the position.
////
Three years after then-President Donald Trump pressured the U.S. National Institutes of Health (NIH) to shut down a research grant to a group studying how bat coronaviruses jump to people, the agency has restarted the award. www.science.org/content/article/news-glance-respiratory-disease-vaccine-intensifying-cyclones-shaking-wood-building?
The new 4-year grant providing $576,000 per year is a stripped-down version of a 2019 grant to the EcoHealth Alliance, a non-profit in New York City. That grant included a subaward to China’s Wuhan Institute of Virology (WIV), which some conservative commentators allege started the COVID-19 pandemic. The restarted grant omits WIV, sampling of bats and people in China, and controversial experiments with live, hybrid viruses. Instead, it funds studies of bat virus’ genomes and characteristics that could cause human disease and lab work with viral proteins and “pseudo viruses” that can’t cause disease. NIH has also imposed extensive new accounting rules on EcoHealth. In January, a federal audit found that EcoHealth had misreported nearly $90,000 in expenses for several grants dating to 2014 and that NIH had erred by not justifying its termination (later changed to a suspension) of the 2019 grant.
////
Lalita Panicker is Consulting Editor, Views and Editor, Insight, Hindustan Times, New Delhi

